
Fat and Fabulous
I was giving a presentation to a group of other doctors and students in the mental health field last week. One attendee interrupted me when I was talking about insulin resistance.
She was probably 100 pounds overweight but told a story that she has already lost about 30 pounds, had decreased her thyroid med dose by 1/3, and even had regression of ovarian cysts. These were fantastic changes and I praised her. She referred to herself as fat and fabulous.
But the part that made her over step her boundaries was her statement that I shouldn’t lump all fat people as unhealthy and that all skinny people are healthy. After all, she was fat (her words not mine) and she is healthy.
First of all, I didn’t; those words never spewed from my mouth nor will they ever. What I was discussing was how certain areas of the body have more or less affinity to store energy (insulin resistance), hence why people gain weight in the butt, gut, and thighs. It’s an area that is a lot less resistant to insulin than the liver or muscles. It’s an easy area to store excess energy.
Then she went on to say how healthy she was and that all her labs came out looking good, etc. I didn’t have time to get into why both of those statements are false in front of the group, so I thought I would tackle it here. She wasn’t looking for my help, just looking to be heard in a crowd.
In my mind, I don’t look at fat as fat. I look at fat as an outward expression of inflammation. You can be fat and fabulous but don’t let that blind you to being inflamed and ignorant.
The fact that she said her labs look good is a huge red flag in my book, especially when she says that other conditions are present, like hypothyroid. Those ‘normal’ ranges on blood work lump 95% of the population as ‘normal’ and fabulous. When I read them, I tighten and interpret those values in a much more narrow spectrum. It ends up being more predictive and preventative in nature.
Secondly, the standard lab work is the epitome of lazy healthcare. I doubt that she was tested for anything of value, especially anything that would be measuring levels of inflammation. If your doctor is only running a TSH to assess thyroid, your cholesterol levels to assess heart disease, or blood glucose to check diabetes, it’s time to go elsewhere.
With that said…
Inflammation
Inflammation is a HUGE word in the health and sickness industry. Everyone is blaming it for something. If Obama is ever feeling down about conservatives blaming him for every problem this nation faces, he should just do a search in PubMed for inflammation. Inflammation is hated upon way more than Obama could ever imagine.
As much as inflammation is a contributor to EVERY disease on the face of the planet, if you couldn’t produce inflammation, you wouldn’t be around long  enough to experience the potential of chronic illness stemming from inflammation.
enough to experience the potential of chronic illness stemming from inflammation.
Your body never does stupid stuff. Your body is always in a state of intelligent adaptation. Sometimes that adaptation is to produce inflammation. Inflammation happens for 2 very life saving, life building reasons.
- Fight Infection and be used as a first line defense. The coughing, sneezing, runny nose, diarrhea, fever, and sweating isn’t the fault of the bug. This is your body’s response to the bug. You sneeze to expel the bug at 35 mph to a distance of 12-20 feet away (according to the Myth Busters duo, who dispelled the 100 mph to 30 feet away sneeze mantra). Suppressing these symptoms with steroids, anti-histamines, and other amphetamine based cold and cough meds just allows the little buggers to stick around longer, keeping you sick longer.
- Injury/Tissue Repair. You work out to get bigger and stronger. You are voluntarily injuring yourself for the purpose of allowing your body to build it back up again. All that soreness you experience the day or 2 after a workout isn’t a build of lactic acid. It’s the damage you created in your workout. You sliced and diced your cells. Inflammation comes in to clean up the debris and recruit factors to rebuild. Again, taking prescription anti-inflammatory compounds like NSAIDS delays your healing and recovery, not to mention destroys your stomach in the process, which in turn creates another reason for inflammation to be activated to heal up another part of the body. This is why I also caution the consumption of caffeine, especially after an injury. Caffeine triggers the adrenals, which releases Cortisol, which has anti-inflammatory effects on the body by suppressing the immune system. The more caffeine, the longer you deal with the injury.
No matter if inflammation is produced to fight infection or repair a torn bicep, it’s all an immune reaction. I’m sure we have all experienced the acute inflammatory process of red skin and swelling. But what I want to dive into is when that short-term process becomes chronic.
Short term, acute inflammation is tissue destruction. Chronic inflammation is tissue dysfunction. That’s why I want to highlight some of the not-so-obvious inflammatory results of being obese. Obesity isn’t the only cause. I’m only highlighting it because of the dilemma between how people perceive beauty versus how people perceive health. You can be big and beautiful; just don’t be inflamed and ignorant.
Inflammation can be triggered from external events or internal events. External events are things like bacteria, virus, as well as allergens, irritants, toxins, and foreign bodies.
Internal events are often from the normal, every day activities of cell turnover than create inflammatory signals. It could be signals from damaged tissue, malfunctioning tissue, and just the normal breakdown of cells. If cells are breaking down faster than programmed, inflammation goes up.
This is where you can use A1C as a good initial indicator of how much stress and damage the body is under going. A1C is more than a marker for sugar utilization. It’s a compound made of a sugar that has attached to a protein (in this case hemoglobin form your red blood cells). The higher your A1C, the more damage is occurring in the body. There are exceptions, but in general, this is a good starting point to quantify damage and if you are improving and preventing excessive damage.
Just like the woman, don’t assume your values are great if they fall within normal. I will flag values over 5.4%. I don’t want to wait until it becomes out ‘normal’ range to take action.
If you have excess weight around your butt, gut, and thighs, you have insulin resistance. BUT, just because you are skinny doesn’t mean you can’t have insulin resistance. I’ve analyzed many ‘skinny’ people that have elevated A1C values.
Along those same lines; if you have pain you have inflammation. BUT, you can be inflamed and have no pain. 1/3 of all heart attacks have the first symptom of death. You can be inflamed and not feel it.
Cytokines
There are some key players in the inflammation game. The players fall under a broad category of proteins called Cytokines. These are released by cells and influence the behavior of cells.
Details get long and boring and distract from the main point. The main point is that when you expand your view of certain conditions, you will approach your health strategy differently.
This may get a little nerdy.
Adipocytes (fat cells) produce a cytokine called IL-6 (Interleukin 6). IL-6 tells the liver to produce other inflammatory responses, both acute and chronic, such as Ferritin, CRP, and Fibrinogen.
CRP is often used in assessing cardiac risk. This is one of those markers that you should ask your doctor to test regularly. I flag a value that is over 0.5 mg/L. CRP is a very sensitive marker for inflammation but not that specific. With that said, it’s not elevated in ALL causes of inflammation. Elevations over 7, are more likely to be acute infections and trauma. Chronic low to moderate levels (0.5 – 7) are more likely chronic and systemic, like heart disease but also auto-immune, neurological disorders, arthritis, and GI problems.
A side note for the ladies. An IUD (Intra-Uterine Device) works by causing inflammation in the uterus and may elevate CRP levels.
A side note for you men. Don’t confuse an IUD with an IED (Improvised Explosive Devise).
CRP attaches to cell membranes to attract immune cells for clean up. The immune system is the inflammatory response. The catch is that CRP is released in response to other inflammatory signals but has the ability to signal for more IL-6. Remember that fat cells produce this IL-6.
Inflammation likes to party. Chronic inflammation is like making love to a gorilla. It doesn’t stop until the gorilla stops.
[bctt tweet=”Chronic inflammation is like making love to a gorilla. It doesn’t stop until the gorilla stops.”]
Most medications are geared at treating the symptoms of inflammation or cutting out one of the links in the inflammation chain. The problem is that people may feel better but until they address the underlying reason that inflammation is being produced, it’s going to be a vicious cycle.
The med cuts out part of an inflammatory response but remember, that response was happening for a good reason. It was there to fight infection or repair tissue. As the medicine lowers that response, the body signals for MORE inflammatory signals in order to keep up with demand to fight or repair. In reality, your anti-inflammatory medication is actually setting you up to be in a more inflamed state.
The other catch 22 is that because the medicine also has effects other than being anti-inflammatory, this creates more damage internally. What happens when damage occurs? Your body activates the immune system to regulate inflammation.
Seasonal Side Note:
As we enter “Flu Season,” how can this information help you? The #1 reason for antibiotic prescription is for Lower Respiratory Tract Infections (LRTI), which are things like persistent cough and bronchitis (accounts for 80% of LRTIs). Despite evidence of little to no benefit of antibiotic treatment for LRTIs, 75% of them will be treated with antibiotics.
With the increase in bacterial resistance and potential side –effects of antibiotics, not to mention the complete disruption of the beneficial bacteria that resides in your gut, you can use CRP as indication to help your doctor to choose if the infection is bacterial or viral.
Side not to men: You can think of antibiotics as an IED on your insides. But again, don’t confuse an IED with an IUD. Don’t give an IUD to your kids if they have pneumonia.
Why do I say you can help your doctor? Because old habits are hard to change. The uncertainty of whether something is bacterial or vial leads to uncertainty for practitioners. When in doubt, they give a script for antibiotics in case it’s pneumonia instead of bronchitis. It isn’t feasible for everyone in a primary care setting to routinely get chest x-rays.
A study in Spain divided groups of practitioners using the same protocol to assess LRTI except that one group was given the use of a rapid CRP test. When CRP was less than 10 mg/L, the odds that antibiotics were going to be used was way less than the group that didn’t have access to the CRP test.
It has been observed that CRP elevates with bacterial infections but not much with viral infections. The cool thing in the study was that the rapid CRP test took about 3 minutes to perform. Other signs and symptoms have to be considered but it was an added tool that proved to lower the action of just throwing antibiotics at an infection that would not have any positive effect.
Seasonal Side Note Done.
Let’s review. Fat cells 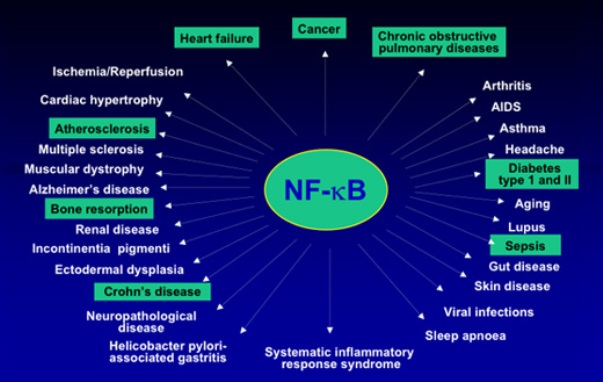 produce IL-6, which tells the liver to produce more CRP, which in turn produces inflammation all over. Inflammation likes to party and signals for the master of ceremonies, NFkB. NFkB is a gene promoter and driver of inflammation.
produce IL-6, which tells the liver to produce more CRP, which in turn produces inflammation all over. Inflammation likes to party and signals for the master of ceremonies, NFkB. NFkB is a gene promoter and driver of inflammation.
You will find elevated levels of NFkB in inflammatory bowel disease, arthritis, sepsis, asthma, atherosclerosis, and many nerve degeneration diseases including schizophrenia. It’s also elevated in many cancers.
All these possible effects just because of a little extra weight in that mid section. Obesity isn’t about judging someone’s beauty. You may think you look fat and fabulous but accepting that and doing nothing will leave you in a world of hurt later down the road. Contentment is fantastic and a major source of stress in the American culture is a lack of contentment. But it doesn’t mean you don’t try to keep improving yourself.
Thyroid Disease: Chicken or the Egg?
Many will be concerned about their thyroid because they are gaining weight. But what if it was the other way around? What if there was already inflammation occurring and the thyroid is being damaged from that?
I have seen hypo-thyroid disorders in skinny people and I have seen hypo-thyroid disorders in fat people. Remember, skinny people can have insulin resistance, it just might not be super visible from the exterior.
What if someone was already heavy or has insulin resistance and because of the IL-6 that the adipose cells produce, this is what was damaging the thyroid? It’s been shown that Interleukins will damage thyroid receptors and cause thyroid resistance.
Much of the literature isn’t about inflammation and thyroid dysfunctional alone. It’s about inflammation, thyroid dysfunction, AND insulin resistance.
See some references at the bottom.
You want to help your thyroid? Stop chasing TSH so much and find the source of inflammation. Remember, inflammation responds due to injury or illness. Therefore, some main causes of inflammation that can affect your thyroid are obesity and insulin resistance (low-fat diets), chronic infection, leaky gut, emotional stress, and pollutants like heavy metals.
You can be fat and fabulous but don’t be inflamed and ignorant.
This is Your Brain On Inflammation…
Remember inflammation likes to party. Cytokines can trigger microglial activation. Microglial cells are your first line of defense in your central nervous system (brain and spinal cord). They are a type of immune cell.
Remember the purpose of inflammation is to seek and destroy. These microglial cells can destroy the next closest nerve cells and/or affect neurotransmitter function. The more this happens, the more an auto-immune condition is set up for the brain and mental/emotional conditions.
As a result, MAO (MonoAmine Oxidase) stimulates the breakdown of serotonin and dopamine. Disruptions in these neurotransmitters will affect behavior, mood, memory, concentration, learning, sleep, appetite, and even addiction.
Inflammation can affect the pituitary, which disrupts the pathway from brain to adrenals. The more adrenals are fired, the more cortisol is released. The more cortisol is released, the more sugar is dumped into the blood stream. The more sugar is present, the more insulin gets released. But because Cortisol is a protective hormone (saves you from a bear) and insulin is a growth hormone (repairs you after the bear attack), cells favor cortisol, and thus insulin resistance ensues. You can’t be in growth and protection at the same time.
One of the lease resistant areas in the body to store excess energy is that area in the butt, gut, and thighs. We’re back to packing on adipose tissue, which releases more interleukins, which promote CRP, and the cycle is happening all over again.
The list of conditions that are affected by inflammation can go on for days. One of the largest areas of inflammation in the body is excessive body fat. Toxins love fatty tissue. The more we are exposed to toxins, the more it’s apt to be deposited in fatty tissues. The toxic burden can add to the interleukin load and add more inflammatory insult to inflammatory injury.
I’m Not Judging…
Please hear me when I say this. Yes, you can be beautiful and obese. But it’s not possible to be healthy and it has nothing to do with you carrying extra weight. It’s what those cells produce that lead to volumes of contributing factors for other disease processes.
And also please hear me when I say, it’s not about dying with less weight. There are a thousand ways to lose weight that also don’t create health.
But do hear me when I say this. You might be having hard time losing weight because of the amount of inflammation happening. Worry about addressing inflammation and weight loss will be a desired side-effect.
Need specific strategies for you? You know how to contact me.


Great goods from you, man. I have bear in mind
your stuff previous to and you’re simply extremely magnificent.
I really like what you’ve received right here, really like what you
are saying and the best way in which you say it. You make it enjoyable and you still take care of to stay it sensible.
I cant wait to read much more from you. That is really a tremendous web site.